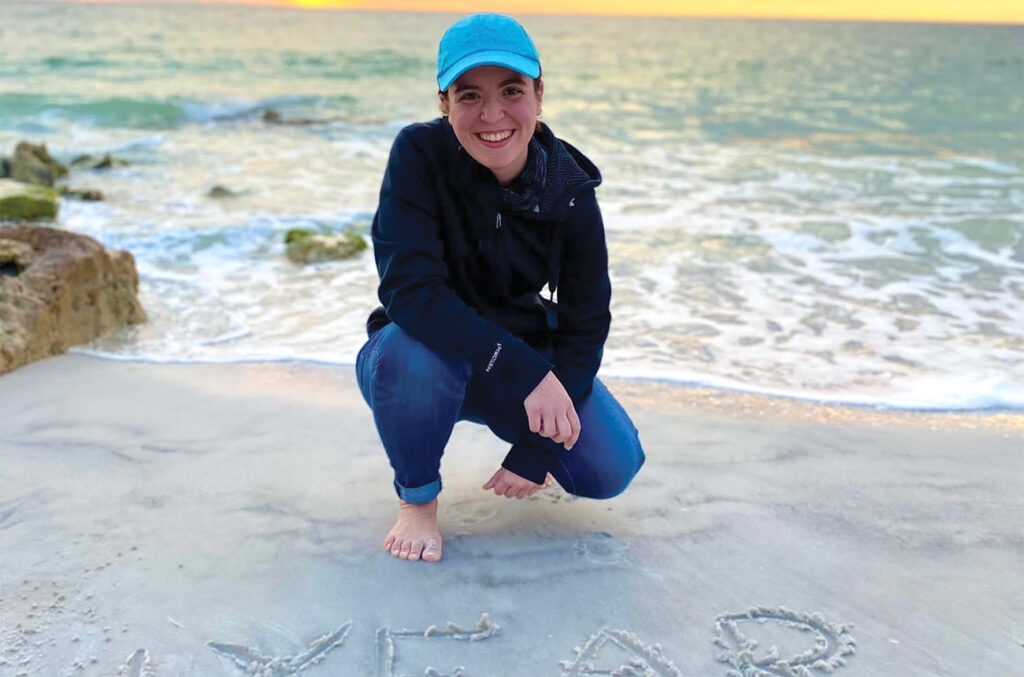Emma Beutow can’t remember life without epilepsy, but her mom Misty recalls the first time Emma had a seizure at age 3. Actually, she didn’t know it was a seizure until later. Like many people, Misty associated seizures with dramatic convulsions. Emma’s seizures were more subtle.
“She would do these weird things where she would stop talking and her stomach would hurt,” remembers Misty. “It was like suddenly she wouldn’t be able to communicate with us.”
Most children who have epilepsy will outgrow the condition, but at 12, Emma was still having seizures. The Beutows lived with the ever-present fear that something would happen. A lively teenager who loved volleyball, Emma sat out many games and practices and was constantly fatigued. Being in the water was dangerous, so Emma avoided pools, lakes, even baths.
When she had a seizure, her memory would go blank. Driving was absolutely out of the question, as was going away for college. Emma assumed her future would entail attending community college and living with her parents.
Thanks to her bravery, and trusting the innovative treatments offered by Washington University surgeons at St. Louis Children’s Hospital, Emma’s future now looks quite different. For over a year now, Emma has enjoyed life seizure-free.
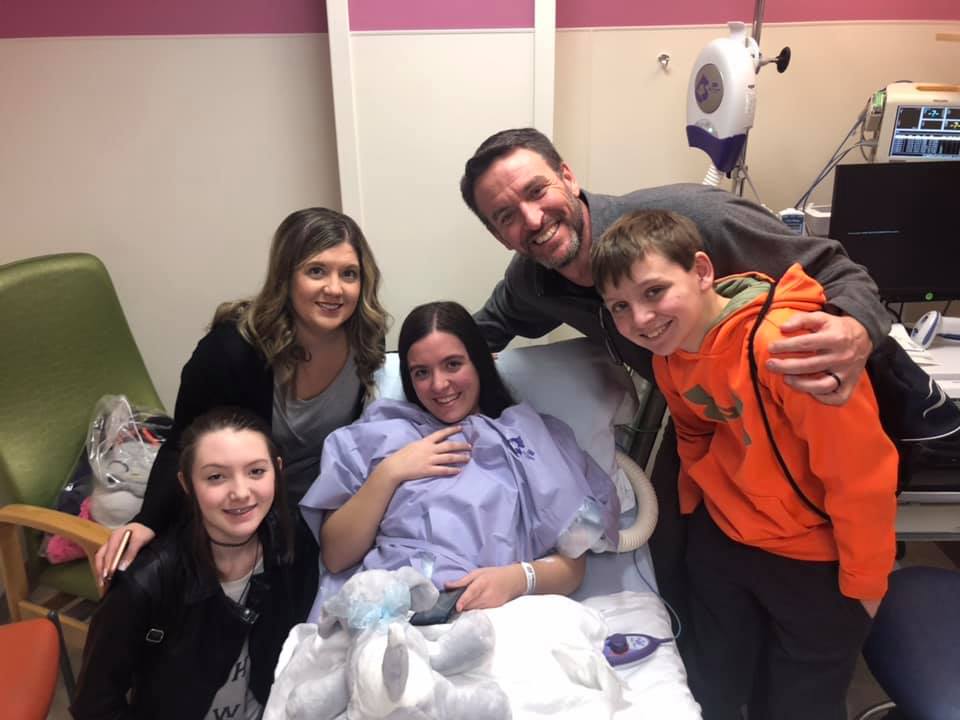
“Now that I’ve gone so long without seizures, I realize how they were impacting me,” says Emma. “I was just so tired all of the time, and I couldn’t do anything. Now when someone asks if I want to do something, I say ‘of course!’”
When it became apparent that Emma would not outgrow her epilepsy, the Beutows’ long-time neurologist in their central-Illinois town encouraged them to seek more advanced treatments with Matthew Smyth, MD, at St. Louis Children’s. A Washington University neurosurgeon, Dr. Smyth, specializes in treating children with epilepsy using the most innovative surgical procedures.
Learn more about pediatric epilepsy care at Washington University »
Music, braids, and brownies—and ROSA the robot
At St. Louis Children’s, the family was immediately impressed by the level of collaboration amongst Emma’s team of doctors and specialists. They felt calmer knowing that Emma’s options were being evaluated by multiple experts with different skills.

Epilepsy can vary greatly depending on the individual, so in order to make the best decisions regarding Emma’s treatment, the team at St. Louis Children’s needed to begin by mapping where in her brain the seizures originated. For this procedure Dr. Smyth and his team used ROSA, a robotic surgical assistant, to place electrodes through small holes drilled in the skull.
Misty felt uneasy seeing her daughter hooked up to wires, but the team of people in charge of Emma’s care softened the experience for her. One of Emma’s favorite nurses braided her hair so it didn’t get in the way of the electrodes, resulting in several fun hairstyles that were so professionally done they stayed in for days.
Later, Emma underwent another exploratory exam called the WADA test, conducted by experts in radiology and neuropsychology, to pinpoint parts of the brain that house critical functions such as memory and language. Requiring that she be conscious, the WADA test was the only procedure that Emma feared.
On the day of her WADA test, Emma was wheeled from her room at St. Louis Children’s to the testing room downstairs. The trip took several minutes, giving her anxiety time to build, but when the elevator doors opened, a musical therapist was waiting to greet her, and she travelled the rest of the way to the sound of guitar music.

For Emma, who is deeply passionate about music and plays six instruments, this seemingly spontaneous burst of song was a blessing.
From the musical moment on the way to surgery, to the therapy dogs who visited her, to the patient coordinators who greeted her by name, Emma felt supported. In fact, she looks back on the days spent in the hospital with a smile, referring to Shannon Dobbs, the Neurosurgery coordinator, like a family friend. Even the hospital food had something going for it — Emma recommends the turkey burger and the brownie to any who find themselves ordering dinner at St. Louis Children’s.
Removing the seizure-causing lesion
After the WADA test came Emma’s first therapeutic surgery — the laser ablation to burn away the brain lesion that caused her seizures. Assisted by the ROSA robot during a live MRI scan, Dr. Smyth threaded laser fibers through the small holes in Emma’s skull. These laser fibers then heated the abnormal patch of brain tissue to ablate, or remove, the seizure onset zone.
When the laser ablation surgery reduced the frequency of Emma’s seizures, but didn’t eliminate them, Emma and her mother asked what other innovative treatments were available. Dr. Smyth explained that they could use a medical device implant called the NeuroPace, one of the newest and most complex technologies available to treat epilepsy
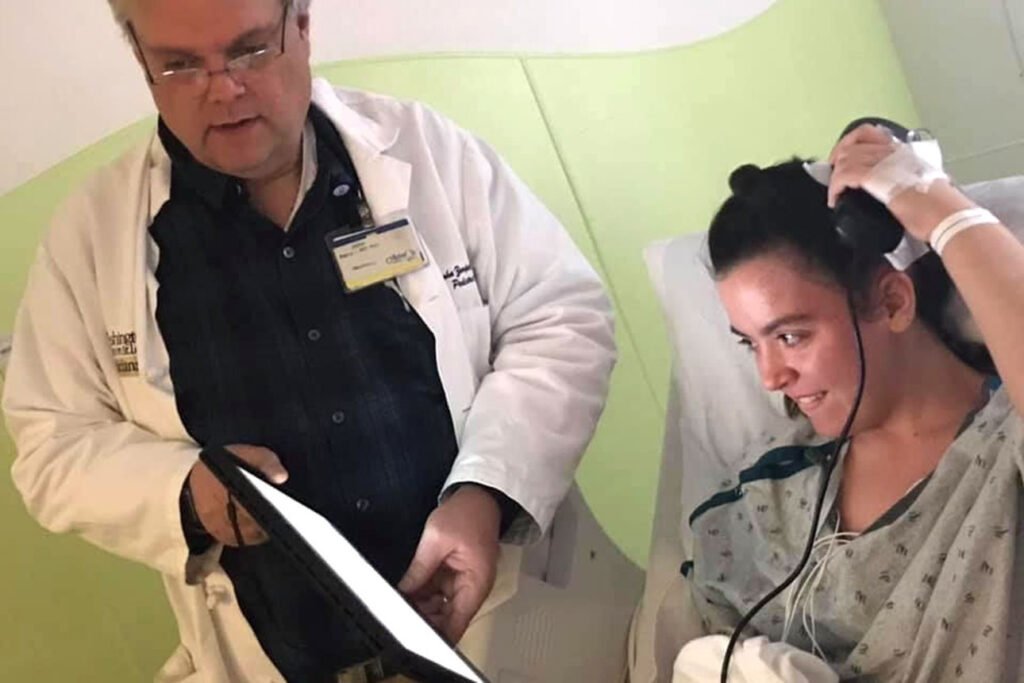
“The NeuroPace is like a pacemaker for the brain with implanted electrodes in the seizure onset zone that detect impending seizure activity and short-circuit the seizures with small pulses of electricity,” according to Dr. Smyth.
Emma embraced the innovation, and once implanted, Dr. Smyth made adjustments to the NeuroPace, customizing it to Emma’s brain.
Freedom she never expected
Emma has just celebrated an entire year without experiencing a single seizure, and her young adult life has opened up to new possibilities. She plans to study worship music at the Moody Bible Institute in Chicago. To encourage others to experience the kind of freedom she now knows, she will continue blogging, as she has since 2013, to raise awareness about pediatric epilepsy.

Emma’s mom Misty urges parents of epileptic children to advocate for their children by seeking out the newest and best treatment available. Sitting next to her smiling daughter in a volleyball uniform, she says emotionally: “Let them live life to the fullest.”