Post-traumatic stress disorder (PTSD) is a condition that develops in some people who have experienced a shocking, scary or dangerous event. People who have PTSD may feel stressed or frightened, have flashbacks, nightmares and severe anxiety, even when they are not in danger.

About one in 11 people will be diagnosed with PTSD in their lifetime, according to the American Psychiatric Association. Yet the only treatment available is medication and psychotherapy, a gradual and long process, which helps some patients learn to manage it, in part by learning to feel safer.
Now there may be hope for patients with PTSD who fail to respond to more conservative therapies.
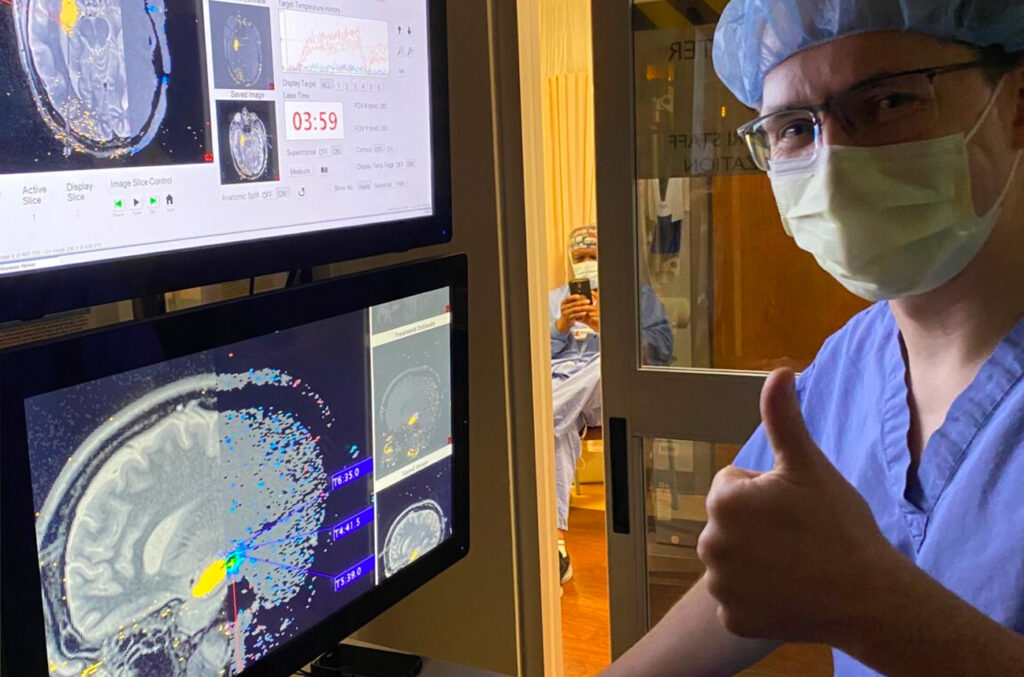
Using a minimally invasive procedure to ablate, or remove, targeted brain tissue, Washington University neurosurgeon Dr. Jon T. Willie and colleagues were able to eliminate PTSD completely for a Vietnam veteran who had suffered PTSD for decades. Using the same procedure, they also successfully treated a civilian PTSD patient who had witnessed extreme violence. Both patients experienced immediate benefits and no longer fulfilled diagnostic criteria for PTSD.
To treat PTSD patients, the key was recognizing that a brain region, the right amygdala, can be the source of persistently abnormal activity that interferes with safety learning. Ablating the right amygdala with a type of heat therapy called laser interstitial thermal therapy (LITT), alleviated excessive fear responses and facilitated safety learning, according to Dr. Willie and colleagues’ research published in Neurosurgery, the official journal of the Congress of Neurological Surgeons. With one amygdala ablated, patients were immediately able to tolerate life events that had previously triggered anxiety, enabling them to engage in safety learning and continue to get better over more than a year of follow up.
Epilepsy patients made possible new PTSD discoveries
To understand where and how to treat PTSD patients, Willie and his colleagues asked patients with epilepsy – and who also had PTSD — if they would participate. Their brains were already being mapped with implanted electrodes to identify where epileptic seizures are coming from.
While mapping seizure onset and spread, the surgeon-scientists recognized that regions of the brain that were contributing to seizures overlapped with the right amygdala, which was hypothesized to also contribute to PTSD. As the right amygdala would be ablated as part of the therapy for epilepsy, the team asked whether PTSD symptoms, as measured by a variety of accepted behavioral, physiological, and functional imaging techniques, would also improve independent of effects on epilepsy. The strategy of studying PTSD incidental to treating epilepsy was necessary since surgery for epilepsy is widely accepted, whereas brain surgery for PTSD is still experimental.
Laser ablation is performed though a small opening in the skull, smaller than the diameter of a pencil. The surgeon uses an MRI to guide the probe which uses laser heat to ablate the region involved in both PTSD and seizures. The method is otherwise the same as that used to treat seizures by advanced epilepsy centers such as Washington University and Emory University, where Willie started this research as a faculty member.
For these two patients, the procedure reduced seizures, and PTSD symptoms were profoundly abated.
Willie has also received a $2.35 million grant from the National Institutes of Health to investigate how to use deep brain stimulation to the amygdala to improve memory and retrain the brain, a process called neuromodulation. If successful, this approach could better enable safety learning in patients with PTSD. He will recruit patients undergoing evaluation for epilepsy surgery including the minority that suffer from both seizures and PTSD. He is also investigating less invasive ways to block abnormal activity in the right amygdala in patients with PTSD alone.