Unable to move her legs and in extreme pain, a woman in her 70s was transferred to Barnes-Jewish Hospital earlier this month. A tumor had invaded her thoracic vertebrae and extended into the spinal canal, crushing her spinal cord and causing her paralysis. Experts at another hospital felt her tumor could not be surgically removed.
“To safely treat patients with complex tumors, we need extreme precision to not only remove the tumor but also reconstruct the weakened spine following the tumor resection,” according to Washington University neurosurgeon Camilo Molina, MD.
Just one day after Dr. Molina removed her spinal tumor at Barnes-Jewish Hospital, the patient was able to move her legs again, even against resistance.
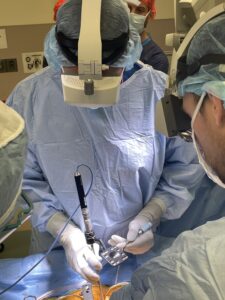
Her prognosis for continued recovery and additional movement is excellent, according to Dr. Molina who completed this complex surgery using a new augmented reality technology called xvision Spine System from Augmedics.
Over the last four years, Dr. Molina has helped develop, test and validate xvision, recently named a Best Invention of 2020 by TIME magazine. Dr. Molina performed the first surgery in the world using this technology in June at The Johns Hopkins Hospital. Washington University is now one of five academic institutions using this new technology.
Augmented reality simulates “x-ray” vision during surgery
Augmedics xvision technology allows surgeons to visualize the patients’ 3D and 2D spinal anatomy during surgery and accurately navigate instruments and implants while looking directly at the patient. This is a departure to prior tools that distracted the surgeon by displaying this navigation data on a remote screen. It’s as if the surgeons have x-ray vision, according to Dr. Molina, who is assistant professor of Neurosurgery and Orthopedic Surgery, as well as deputy director of Spine Innovation for the Center for Innovation in Neuroscience and Technology at Washington University.
“Dr. Molina’s development and now clinical use of this exciting and innovative technique for making spine surgery safer and more effective for our patients is truly inspiring.”
Gregory J. Zipfel, MD, chair of the Department of Neurosurgery at Washington University School of Medicine
With other mapping technologies, surgeons look at a screen, not the patient, while placing instrumentation, Molina explained. In the case of xvision, the surgeon wears a headset that incorporates all the navigational information from the patient’s CT scan.
It’s the difference between driving and looking down for directions and driving with the GPS translucently on the windshield in front of you like modern cars with heads-up-displays. Older technologies require cameras around the patient, and occasionally those cameras become blocked by movement in the room – losing their navigational capacity. Because the camera tracking for the xvision occurs on the head of the surgeon, the surgeons’ computer navigation is never blocked.
Seeing the anatomy precisely, along with the exact location of the surgical tools and implants throughout the surgery, was particularly important for the success of our patient’s complex surgery, according to Molina.
Because of the depth of the tumor, the surgery required removing an entire vertebra that had the tumor in it and then putting a metal cage implant where the vertebra used to be, using screws and rods to connect to the other vertebra to restore the structural integrity of the spine.
The other challenge was taking the tumor off the neural elements. Given the patient’s age and condition, this “big surgery required a minimally invasive approach,” said Dr. Molina. The xvision augmented reality tool enabled the surgeon to put all the rods and eight screws in through the skin, without opening her entire back.
The purchase of the Augmedics xvision technology was funded by the Foundation for Barnes-Jewish Hospital and the generosity of the foundation’s donors.